 In the low birthweight infant, the level is proportionately lower. The specific serum level of unconjugated bilirubin that results in kernicterus is unknown, but for the term infant it has traditionally been defined as a concentration of 20 mg/dl. When the serum level of unconjugated bilirubin exceeds the albumin binding capacity, bilirubin diffuses into the central nervous system and may result in permanent neurological damage or death (bilirubin encephalopathy with kernicterus).Ĭonjugated bilirubin is water soluble and does not diffuse into the central nervous system so it is not capable of causing kernicterus.įactors such as acidosis and hypoalbuminemia may reduce the ability of albumin to bind to conjugated bilirubin. 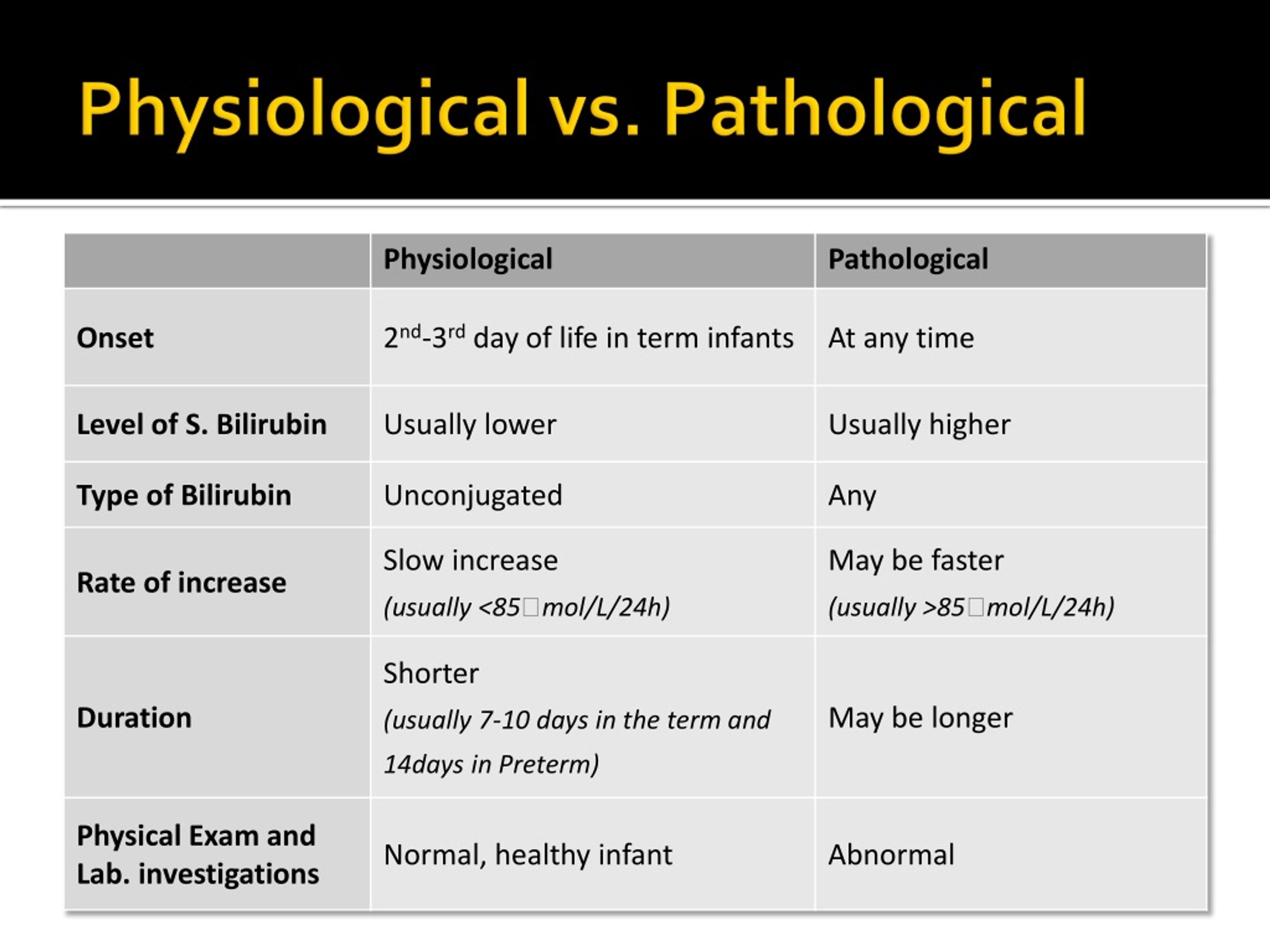
The level of glucuronyl transferase is initially low in the newborn and any increase in the rate of bilirubin formation can overwhelm the capacity to conjugate, thus resulting in elevated bilirubin levels. Most unconjugated bilirubin is excreted in the stool, but some is reabsorbed and returned to the liver for re-conjugation (enterohepatic circulation). In the small bowel, some of the bilirubin is hydrolyzed to yield unconjugated bilirubin and glucuronic acid. Conjugated bilirubin is secreted into the bile and enters the duodenum. Unconjugated bilirubin is bound to albumin in the plasma and transported bound to albumin to the liver and is conjugated with glucuronic acid in the hepatocytes the conjugation is catalyzed by glucuronyl transferase. Heme is catabolized to unconjugated bilirubin in the reticuloendothelial system. Excessive bruising from birth trauma or abnormal blood collections such as in a cephalohematoma may further add to the rate of RBC destruction and bilirubin formation. Bilirubin is a yellow substance your body creates when red blood cells break down. Hyperbilirubinemia is the medical term for this condition. Jaundice occurs when bilirubin (pronounced bil-ih-ROO-bin) builds up in your baby’s blood. The rate of neonatal RBC destruction is higher than in adults resulting in greater quantity of hemoglobin release. Overview What is jaundice in newborns Jaundice in newborns is the yellow coloring in an infant’s skin. In newborns, the normal hemoglobin level is 15-18 mg/dl. Red cell hemoglobin accounts for approximately 85% of all bilirubin.  
Bilirubin Metabolismīilirubin is a product of heme catabolism. Serum bilirubin levels in pathological jaundice must be greater than 225 mcmol/L. The most common cause of pathological jaundice is the G6PD deficiency. Pathological jaundice appears 24 hours after birth. Although neonatal hyperbilirubinemia is usually a benign and physiologic condition, very high bilirubin levels occur in certain pathologic conditions and are potentially injurious to the central nervous system. Newborn Pathological Jaundice True or False: Conclusion: Quiz 1. After 24 hours, visual assessments should. Jaundice is seen in approximately half of all newborns. The transcutaneous bilirubin or total serum bilirubin level should be measured immediately if infants are noted to be jaundiced within 24 hours of birth. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
